What is the prostate
The prostate is a walnut-sized gland and an important part of the male reproductive system. It is located just below the urinary bladder, and one of its functions is to produce semen.
As men age, the prostate undergoes changes such as increasing in size, a common condition known as benign prostate hyperplasia (BPH), or uncontrolled cell growth which can become malignant and lead to prostate cancer.
What is Prostate Cancer?
Prostate cancer is a type of cancer that begins in the gland cells of the prostate.
According to statistics from the Singapore Cancer Society, prostate cancer is the second most common cancer among Singaporean men, especially those above the age of 50.
What causes prostate cancer
While it is unclear why this happens, doctors know that it begins when prostate cells undergo genetic changes. This leads to rapid and abnormal growth and division of cells which form a malignant tumour. These cancerous cells then invade surrounding tissue such as the seminal vesicles and bladder neck.
Signs and symptoms of prostate cancer
In most cases, prostate cancer develops without any visible symptoms. This makes detection difficult and the cancer may spread through the body’s lymphatic system and into other parts of the body such as the lungs. It can also spread to lymph nodes in the pelvis or to the bones.
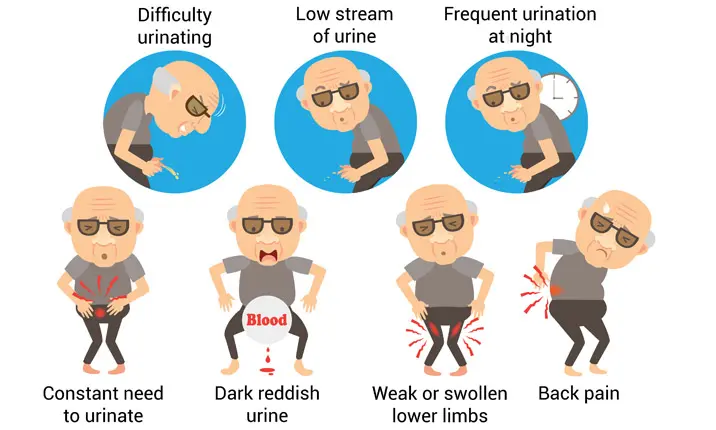
Some symptoms of prostate cancer include:
- Constantly feeling the need to urinate
- Feeling a strong need to urinate, but having a very low stream of urine
- Frequent urination at night
- Dark, reddish coloured urine
- Difficulty urinating
- Weakness or swelling of the lower limbs
- Back pain, especially at rest/at night
If you experience any of these symptoms, you should seek advice from a doctor.
Risk factors for prostate cancer
There are several factors that increase your risk for developing prostate cancer. These include:
- Increasing age, as prostate cancer is more common in men above 50 years
- Ethnic background, with prostate cancer significantly more common among Chinese men in Singapore compared to other ethnic groups
- Family history of prostate cancer or breast cancer
- Obesity, with some studies finding that cancer in obese persons is more likely to be aggressive and to return after treatment
Testing for prostate cancer
As most prostate cancers do not cause symptoms in the initial stages, men who are concerned about prostate cancer can speak to their doctors about testing for early prostate cancer. This can be considered when men reach 50 years of age, or earlier if they have a family member with prostate cancer.
There are several tests your doctor may recommend to detect prostate cancer.
Types of prostate cancer test
Digital rectal examination (DRE)
In a digital rectal exam, your doctor will insert a gloved and lubricated finger into the rectum to feel for abnormalities such as enlarged or hardened areas of the prostate.
Prostate-specific antigen (PSA) test
The prostate produces a specific antigen which is normally present in small quantities. Changes in the prostate, such as enlargement, infection or cancer, can cause higher levels of prostate-specific antigens measured in a blood test.
A PSA is often recommended as a screening test for those who may not exhibit any symptoms. While there is no specific level that determines whether a patient has prostate cancer or not, those with PSA levels between 4 – 10ng/mL of blood are estimated to have a 1-in-4 chance of having prostate cancer. For those whose levels are between 10-20ng/ml, the chance of finding prostate cancer is 30-50%. The risk of finding prostate cancer gets higher with higher PSA levels.
For men who have already been diagnosed with prostate cancer, a PSA test may be performed to help your doctor determine the stage and grade of the cancer, so that an appropriate treatment regimen can be advised.
Prostate Health Index (PHI)
The PSA test has a limited specificity to detect prostate cancer, especially in the grey zone of PSA 4-10ng/ml. This may result in men undergoing unnecessary further testing.
The Prostate Health Index (PHI) is a blood test that is more specific than a PSA, and helps further risk-stratify men at risk of prostate cancer. This test can reduce the risk of unnecessary prostate biopsies.
MRI Prostate
If there is a suspicion for prostate cancer, MRI of the prostate may detect suspicious areas which can then be targeted during a prostate biopsy. On the other hand, if the MRI does not show any suspicious areas, your doctor may recommend further observation instead.
Prostate biopsy
If a DRE and/or PSA test reveal abnormalities, a biopsy may be recommended to collect tissue samples so they can be checked for cancer.
In this procedure, a needle will be inserted into the prostate either through the rectum in a transrectal biopsy, or via the skin between the anus and scrotum in a transperineal biopsy. This may be repeated several times so that the doctor can collect samples systematically from different parts of the prostate. The transperineal biopsy has the advantage of a lower risk of post biopsy infection and bleeding from the rectum compared to the transrectal biopsy.
Systematic biopsy is a blind procedure, where your doctor is unable to see the suspicious areas within the prostate while collecting the sample. Therefore, several samples are taken to improve the chances of detecting cancer if it is present. The samples will then be checked in a laboratory.
Systematic biopsies have a false positive rate of 25-30%, meaning a negative biopsy result does not exclude cancer, and that further follow-up may be required.
If a MRI prostate was done beforehand, the information from the MRI can be used to aid in targeting the suspicious areas. In this way, targeted biopsies are more accurate than systematic biopsies, leading to more certainty after the biopsy.
Thus transperineal MRI-guided targeted prostate biopsy is the current cutting-edge technology for prostate biopsies.
Early screening for prostate cancer can reduce the risk of death. And the sooner treatment commences, the higher the chances of positive outcomes and recovery.
Read more about why you should test for prostate cancer early here.
Understanding your prostate biopsy results
A prostate biopsy will reveal 1 of 3 results:
- Negative for cancer, which means that no cancer cells were found in the samples. As there is a chance of false-negative results, your doctor may advise a repeat biopsy or other tests should there be a strong suspicion of prostate cancer based on your risk factors and/or symptoms.
- Positive for cancer, which means that cancer cells were found in the samples. A grade will be assigned, with higher grades of cancer indicating that the cancer is more likely to grow and spread quickly.
- Suspicious, which means that something abnormal was found, and it is unclear whether it may be cancer or not. Your doctor will advise if further tests are needed to rule out cancer or other conditions.
Types of prostate cancer treatment
Your doctor will recommend an appropriate treatment for you, which may include 1 or more of the following:
Radical prostatectomy
A radical prostatectomy is the surgical removal of the prostate. In Singapore, this is most commonly performed with the assistance of a robot-assisted surgical system. This tool gives the surgeon magnified vision, with small wristed instruments that replicate the dexterity of the surgeon’s own hand, allowing the surgeon to precisely remove the prostate through small incisions of 1cm or less. Through robotic assisted radical prostatectomy, patients typically experience less pain from smaller incisions, less blood loss and shorter hospital stays (usually 2 nights), compared to open surgery.
Radiotherapy
Radiotherapy involves the use of high-energy x-ray beams targeted at the prostate from outside the body. These x-ray beams damage the cancer cells and stop them from growing and spreading to other parts of the body.
Other treatment options
In some cases, some doctors may advise you to wait, as not all prostate cancers need to be treated immediately. Some cancers progress very slowly and thus have a very low potential to cause death. In such situations, your condition can be monitored through regular PSA testing, MRI scans and biopsies. This is called active surveillance, to prevent the need of incurring unnecessary treatment costs or risks for men with cancers that are not likely to harm them.
Read more about various prostate cancer treatment options here.
Early detection and survival rates for prostate cancer patients
Survival rates for prostate cancer depend on several factors, such as the patient’s age and overall health, and the stage or grade of the cancer. As with many types of cancer, early detection and prompt treatment can improve your chances of successful treatment and improve survival rates.
The Singapore Cancer Society reports that, in those with localised disease that has not spread to other organs and low cancer grades, there is a 5-year survival rate for more than 95% of patients.
In those with advanced or metastatic prostate cancer, which means it has spread to other organs, the 5-year survival rate drops to 30%. However, the prognosis for men with advanced cancer has steadily improved with advancements in drug therapy.
To improve your chances of early detection and treatment, experts recommend regular screening to help detect signs of prostate cancer, especially among those with risk factors.
If you have any questions or concerns about prostate cancer, speak to a urologist.