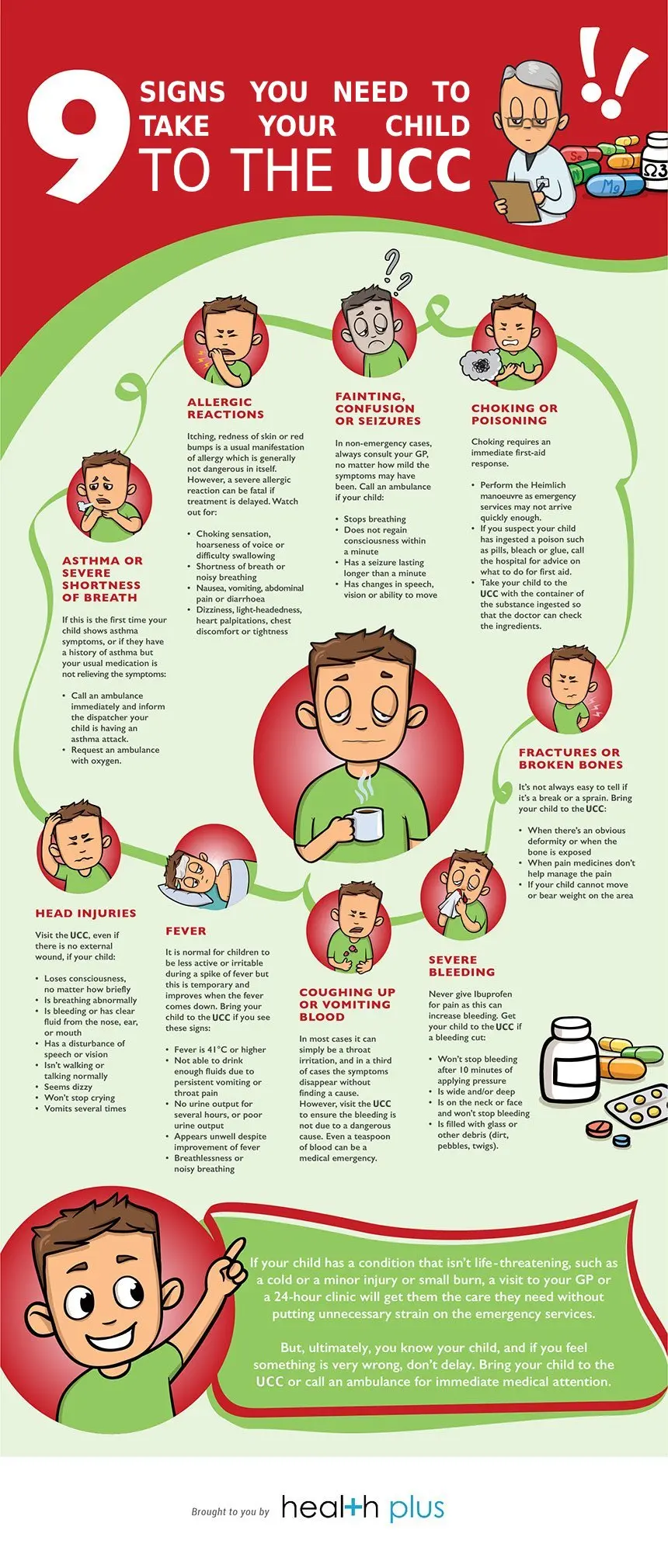
When your child is sick or injured, it's natural for you to worry. Should you call the emergency services or wait to see your GP? Are you overreacting or not doing enough? Here are 9 occasions and warning signs you should proceed to the Urgent Care Centre (UCC):
Allergic reactions
Itching, redness of skin or red bumps is a usual manifestation of allergy which is generally not dangerous in itself. However, a severe allergic reaction can be fatal if treatment is delayed. Watch out for:
- Choking sensation, hoarseness of voice or difficulty swallowing
- Shortness of breath or noisy breathing (wheezing / stridor)
- Nausea, vomiting, abdominal pain or diarrhoea
- Dizziness, light-headedness, heart palpitations, chest discomfort or tightness
Asthma or severe shortness of breath
If this is the first time your child shows asthma symptoms, or if they have a history of asthma but your usual medication is not relieving the symptoms:
- Call an ambulance immediately and inform the dispatcher your child is having an asthma attack.
- Request for an ambulance with oxygen.
Fever
It is normal for children to be less active or irritable during a spike of fever but this is temporary and improves when the fever comes down. Bring your child to the UCC if you see these signs:
- Fever is 41°C or higher
- Not able to drink enough fluids due to persistent vomiting or throat pain
- No urine output for several hours, or poor urine output
- Appears unwell despite improvement of fever
- Breathlessness or noisy breathing
Choking or poisoning
Choking requires an immediate first-aid response.
- Perform the Heimlich Manoeuvre as emergency services may not arrive quickly enough.
- If you suspect your child has ingested a poison such as pills, bleach or glue, call the hospital for advice on what to do for first aid.
- Take your child to the UCC with the container of the substance ingested so that the doctor can check the ingredients.
Coughing up or vomiting blood
In most cases it can simply be a throat irritation, and in a third of cases the symptoms disappear without finding a cause. However, you need to visit the UCC to ensure the bleeding is not due to a dangerous cause. Even a teaspoon of blood can be a medical emergency.
Fainting, confusion or seizures
In non-emergency cases, always consult your GP, no matter how mild the symptoms may have been. Call an ambulance if your child:
- Stops breathing
- Does not regain consciousness within a minute
- Has a seizure lasting longer than a minute
- Has changes in speech, vision or ability to move
Fractures or broken bones
It's not always easy to tell if it's a break or a sprain. Bring your child to the UCC:
- When there's an obvious deformity or when the bone is exposed
- When pain medicines don't help manage the pain
- If your child cannot move or bear weight on the area
Head injuries
Visit the UCC, even if there is no external wound, if your child:
- Loses consciousness, no matter how briefly
- Is breathing abnormally
- Is bleeding or has clear fluid from the nose, ear, or mouth
- Has a disturbance of speech or vision
- Isn't walking or talking normally
- Seems dizzy
- Won’t stop crying
- Vomits several times
Severe bleeding
Never give ibuprofen for pain as this can increase bleeding. Get your child to the UCC if a bleeding cut:
- Won't stop bleeding after 10 minutes of applying pressure
- Is wide and/or deep
- Is on the neck or face and won't stop bleeding
- Is filled with glass or other debris (dirt, pebbles, twigs, etc)
If your child's condition isn't life threatening, such as a cold or a minor injury or small burn, a visit to your GP or a 24-hour clinic will get them the care they need without putting unnecessary strain on the emergency services.
But, ultimately, you know your child, and if you feel something is very wrong, don't delay. Bring your child to the UCC or call an ambulance for immediate medical attention.