Parkway Shenton









Our services
Why choose Parkway Shenton?

Holistic and affordable care centred around you and your family’s needs.
With over 38 clinics around Singapore, there’s always a Parkway Shenton clinic near you.
Access over 1,500 specialists from Gleneagles, Mount Elizabeth, and Parkway East Hospitals.
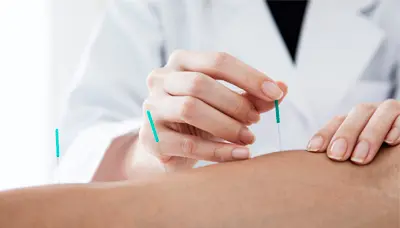
Get prompt treatment and follow-up care for minor surgeries, wound management and more.
Your trusted primary care provider since 1973.
Parkway Shenton clinics are located islandwide
Government schemes and subsidies available

Pay subsidised rates for treatment if you are a Community Health Assist Scheme (CHAS), Merdeka Generation (MG) or Pioneer Generation (PG) cardholder. You can receive treatment for common illnesses and selected chronic conditions at any of our accredited clinics.